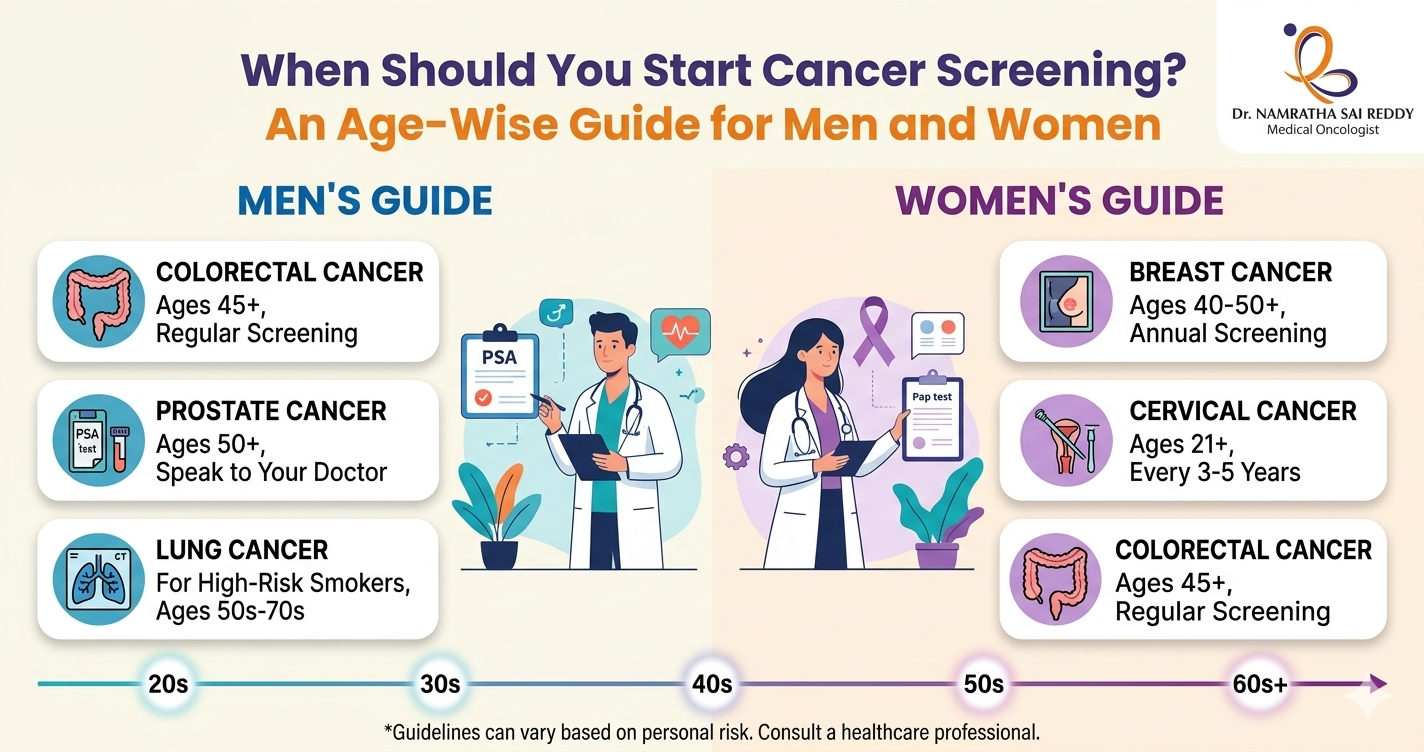
• Most cancer screenings begin between the ages of 21 and 50. Missing or delaying them is one of the biggest reasons cancers go undetected until they’re harder to treat.
• Women start cervical screening at 21, mammograms at 40; everyone starts colorectal screening at 45; men discuss prostate screening at 50. Knowing your age-based schedule removes the guesswork.
• Pap smears and colonoscopies can catch and remove precancerous cells before they turn malignant, making them true prevention tools.
• Family history, genetic mutations (BRCA, Lynch syndrome), smoking, or prior precancerous conditions can move your screening start date earlier. Talk to your doctor if any of these apply.
• Regular screening, even when you feel completely fine, is what makes early detection possible.
Cancer screening should begin at age 21 for women (cervical cancer) and age 45 for both men and women (colorectal cancer). Women should start mammograms at 40, and men should discuss prostate screening at 50. The right age depends on cancer type, gender, and personal risk factors.
Cancer often develops silently, without obvious symptoms in its early stages. That is why screening plays a crucial role in preventive healthcare. Cancer screening tests help detect abnormal cells or early-stage cancers before symptoms appear, allowing treatment to begin when it is most effective.
Why Cancer Screening Is Important
Cancer screening helps detect disease before symptoms appear. Early detection significantly improves treatment outcomes and survival rates. Most early-stage cancers have survival rates of 80 to 90 percent, while advanced-stage cancers are far more difficult to treat.
According to the AACR Cancer Progress Report 2024, overall cancer death rates in the United States fell by 33 percent between 1991 and 2021, translating to an estimated 4.1 million lives saved, a trend driven in large part by earlier detection through screening.
Screening also identifies precancerous changes, allowing doctors to treat them before cancer develops. For example, colonoscopies and Pap tests can prevent certain cancers entirely, not just detect them early.
Key benefits of cancer screening include:
• Early diagnosis and timely treatment
• Improved survival rates
• Less aggressive treatment options
• Better quality of life
• Prevention of certain cancers
Ages 21 to 29: Early Preventive Screening
In this age group, routine screening begins primarily for women.
For Women
Cervical Cancer Screening
Women should begin Pap smear screening at age 21, regardless of sexual activity. The recommended schedule is a Pap test every three years between the ages of 21 and 29. Pap tests detect abnormal cervical cells that may eventually develop into cervical cancer.
Breast Awareness
Women should begin monthly breast self-examinations from age 20 and consult a doctor if they notice lumps, breast pain, or changes in breast shape or skin.
For Men
Routine cancer screening is not typically recommended for most men in this age group unless there are specific risk factors. Men should still attend regular health check-ups that include general examinations for skin changes, lumps or swelling, and abnormal growths. Men with a strong family history of cancer may require earlier screening discussions with their doctor.
Ages 30 to 39: Expanding Screening
In your thirties, screening continues for cervical cancer and preventive health evaluations.
For Women
Cervical Cancer
Women aged 30 to 65 should undergo either a Pap smear plus HPV test every five years, or a Pap smear alone every three years. HPV testing helps detect high-risk strains of human papillomavirus, which are responsible for approximately 99 percent of all cervical cancers.
Breast Cancer
Routine mammograms are not yet recommended for average-risk women in their thirties. Those with a family history, BRCA gene mutation, or other elevated risk factors should discuss earlier screening with their doctor.
For Men
Routine screening is still limited at this age. Men should monitor their health and consult a doctor if they notice persistent fatigue, unexplained weight loss, or lumps and unusual swelling. Men with genetic or family cancer risk may require earlier screening discussions.
Ages 40 to 49: An Important Screening Stage
Cancer screening becomes more structured during this decade.
For Women
Breast Cancer
Women should begin annual mammograms starting at age 40. Mammography can detect breast cancer before symptoms appear, significantly improving survival rates. Thanks in part to early mammography, most breast cancers today are diagnosed at stage I, which carries a five-year survival rate of close to 100 percent.
Cervical Cancer
Continue screening with a Pap plus HPV test every five years, or a Pap test alone every three years.
For Men (High Risk)
Prostate Cancer
Men with increased risk, such as a family history of prostate cancer or of African American descent, should discuss screening with their doctor starting at age 45. Screening may include a PSA (prostate-specific antigen) blood test and a digital rectal examination (DRE).
For Both Men and Women
Colorectal Cancer
Routine screening for colorectal cancer should begin at age 45 for most adults. Thanks to screening, colorectal cancer death rates have fallen by 47 percent in men and 44 percent in women over recent decades.
Ages 50 to 64: Comprehensive Cancer Screening
In your fifties and early sixties, screening becomes essential across multiple cancer types.
For Women
Women should continue annual mammograms. Cervical cancer screening continues with a Pap plus HPV test every five years, or a Pap smear every three years.
For Men
Prostate Cancer
Men aged 50 and above should discuss prostate cancer screening with their doctor. Testing may include a PSA blood test and a digital rectal exam. Shared decision-making, weighing the potential benefits and harms of screening is recommended.
For Both Men and Women
Colorectal Cancer
Recommended screening methods include a colonoscopy every ten years, annual stool tests (FIT or FOBT), flexible sigmoidoscopy every five years, or a stool DNA test every three years. Colonoscopy remains the gold standard because it can both detect and remove precancerous polyps during the same procedure.
Lung Cancer
Adults aged 50 to 80 with a heavy smoking history like 20 pack-years or more, who currently smoke or quit within the past 15 years should receive an annual low-dose CT (LDCT) scan. Despite this recommendation, only around 13 percent of eligible adults are currently up to date with lung cancer screening, the lowest rate of any recommended cancer screening test.
Age 65 and Above: Individualised Screening
Screening decisions after age 65 depend on overall health, life expectancy, and the results of previous tests. Always discuss with your doctor before stopping any screening programme.
For Women
Women aged 65 to 74 may continue annual mammograms or switch to every two years based on personal preference and medical advice. Cervical cancer screening can typically stop after age 65 if previous tests have been consistently normal.
For Men
Prostate cancer screening decisions should consider life expectancy, overall health, and the patient’s own preferences. There is no fixed cut-off age, but screening is generally less beneficial as men age and other health conditions become more significant.
For Both Men and Women
Colorectal cancer screening is usually recommended until age 75, with individualised decisions made after that point. Lung cancer screening may continue for older adults with a significant smoking history and good overall health.
Skin Cancer: Screening for Everyone at Every Age
Skin cancer is the most commonly diagnosed cancer in the United States. Unlike most cancers, there is no fixed starting age, anyone should consult a doctor if they notice new or changing moles, irregular borders, multiple colours within a lesion, or a lesion that is growing or bleeding. Regular annual skin examinations by a dermatologist are recommended for people with a personal or family history of skin cancer, or with significant sun exposure.
Who Should Start Cancer Screening Earlier?
Standard age guidelines apply to average-risk adults. Certain individuals may require earlier or more frequent testing. Higher-risk groups include people with a close family history of cancer, known genetic mutations such as BRCA1/2 or Lynch syndrome, a personal history of smoking or heavy alcohol use, prior precancerous conditions, obesity, or long-term inflammatory conditions such as Crohn’s disease or ulcerative colitis.
Doctors use these factors to create personalised screening schedules, so it is worth raising them proactively at your next appointment.
Warning Signs That Should Never Be Ignored
Do not wait for a scheduled screening if you experience any of the following. Seek medical advice promptly:
• Unexplained weight loss
• Persistent or unusual fatigue
• Lumps or swelling anywhere on the body
• Changes in bowel or bladder habits
• A persistent cough lasting three weeks or longer
• Unusual bleeding or discharge
• Changes in skin moles or lesions
• Difficulty swallowing
Don’t Wait for Symptoms – Start Screening at the Right Age
Cancer screening is one of the most powerful tools in preventive healthcare. Following age-appropriate guidelines can help detect cancers before symptoms develop, dramatically improving survival rates and reducing the need for aggressive treatment.
The data is clear: overall US cancer death rates have fallen by 33 percent since 1991, with an estimated 4.1 million lives saved, a result driven in large part by earlier detection through screening.
Regular screening, combined with healthy lifestyle choices and routine medical check-ups, gives you the best possible foundation for long-term health. If you are unsure when to begin, or whether your risk factors mean you should start sooner, speak with your healthcare provider to create a personalised cancer screening plan.
FAQs
At what age should cancer screening begin?
It depends on the cancer type. Cervical screening starts at 21 for women, mammograms at 40, colorectal screening at 45 for everyone, and prostate screening discussions at 50 (or 45 for high-risk men).
When should women start mammograms?
At age 40 for average-risk women. Those with a family history or BRCA gene mutation may need to start earlier; check with your doctor.
When should men begin prostate cancer screening?
At age 50 for average-risk men, or age 45 if there is a family history of prostate cancer or other high-risk factors.
When should colon cancer screening start?
At age 45, for both men and women. A colonoscopy every ten years is the gold standard, though annual stool tests and stool DNA tests every three years are valid alternatives.
How often should Pap smears be done?
Every three years for women aged 21–29. From 30–65, either a Pap plus HPV co-test every five years or a Pap alone every three years. Screening can stop after 65 if all prior results were normal.
Who should get lung cancer screening?
Adults aged 50–80 with a 20+ pack-year smoking history who currently smoke or quit within the last 15 years should get an annual low-dose CT scan.
Can cancer screening prevent cancer?
Yes, for some cancers. Pap tests and colonoscopies can detect and remove precancerous changes before cancer develops. For others, such as breast and lung, screening catches cancer early when it is most treatable.