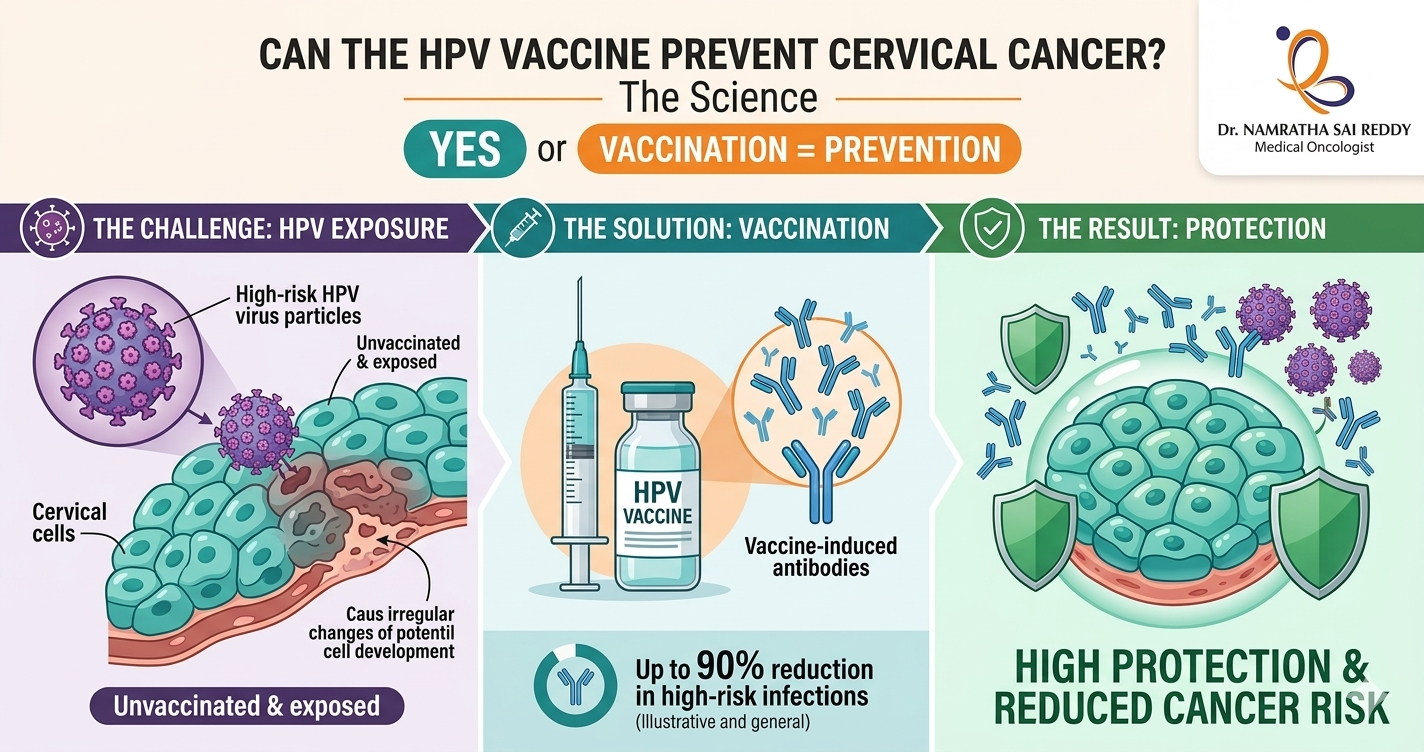
Yes, and the evidence is overwhelming. HPV vaccination reduces cervical cancer risk by up to 88–90% when given before age 17. In India, where a woman dies of cervical cancer every seven minutes, the HPV vaccine is not just a health tool; it is a national emergency intervention. India launched its nationwide free vaccination programme on 28 February 2025, targeting 11.5 million girls aged 14.
Key Takeaways
• India carries the world’s highest cervical cancer death toll. Over 79,906 women died from cervical cancer in India in 2022, more than 22% of all global deaths and a new case is diagnosed every four minutes.
• HPV causes virtually all cervical cancers in India. HPV types 16 and 18 alone account for 76.7% of cervical cancer cases in India, making targeted vaccination extraordinarily effective.
• Early vaccination delivers the strongest protection. Girls vaccinated before age 14 need only 2 doses and gain up to 90% risk reduction. Waiting until adulthood significantly reduces the vaccine’s benefit.
• India now has an affordable home-grown vaccine. CERVAVAC by the Serum Institute of India costs ₹1,400–2,500 per dose in private clinics — and is free at government centres for eligible girls under the national programme.
• Vaccination and screening must go together. The HPV vaccine does not protect against all high-risk strains. Regular Pap smears or HPV DNA tests remain essential, yet India’s current cervical cancer screening rate is just 2%.
The Link Between HPV and Cervical Cancer
Human Papillomavirus (HPV) is the most common sexually transmitted infection worldwide. While most HPV infections clear on their own, certain high-risk strains can persist and cause cancers of the cervix, vagina, vulva, penis, anus, and throat.
Cervical cancer is the most common HPV-related cancer in women. According to the WHO’s Global Strategy for Cervical Cancer Elimination (2025), approximately 660,000 new cases and 350,000 deaths occurred in 2022 alone, with the highest burden in low- and middle-income countries. In India, cervical cancer claims one woman’s life every eight minutes and accounts for approximately 1.23 lakh new cases per year.
Approximately 99.7% of all cervical cancers are caused by untreated or chronic HPV infection, making it one of the most preventable of all cancers. HPV types 16 and 18 alone are responsible for around 70% of all cervical cancer cases globally.
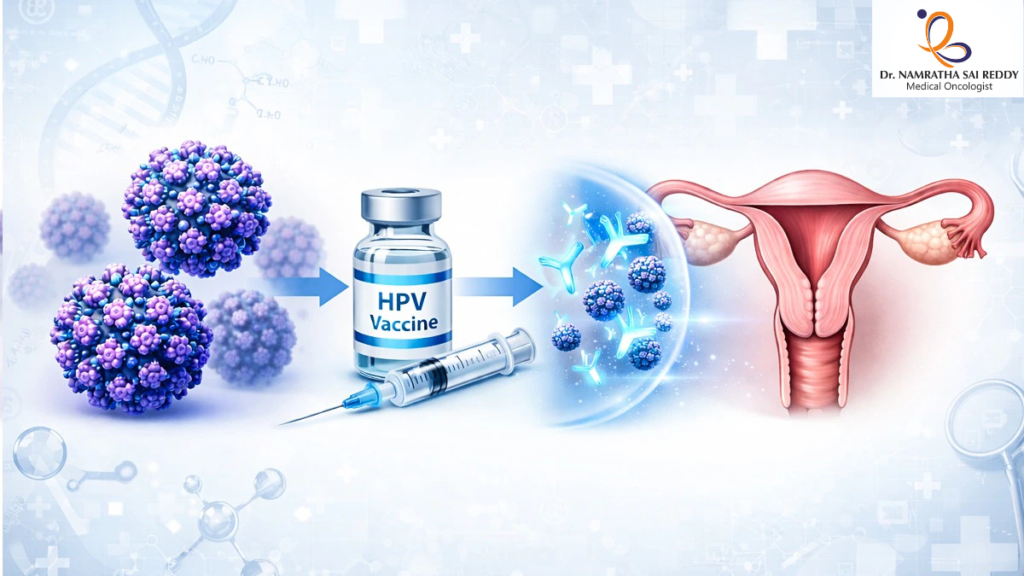
How the HPV Vaccine Prevents Cervical Cancer
The HPV vaccine is a preventive injection, not a treatment. It works by training your immune system to recognise specific high-risk HPV strains before exposure. When a vaccinated person later encounters the virus, their immune system neutralises it before it can establish a persistent infection that leads to cancer.
Think of it as the only shot specifically designed to prevent cancer. The HPV vaccine is not just a vaccine against a virus; it is a vaccine against cancer.
The “shot to prevent cervical cancer” and the “injection to prevent cervical cancer” both refer to the HPV vaccine, available in India as Gardasil, Gardasil 9, Cervarix, and CERVAVAC. It is administered as an intramuscular injection into the upper arm.
HPV Vaccine Types Available in India
As of 2025, India has four approved HPV vaccines. Each differs in the number of HPV strains covered, the approved age range, and cost.
Gardasil 9 (Nonavalent)
• Strains covered: HPV 6, 11, 16, 18, 31, 33, 45, 52, 58 (9 strains)
• Age range: 9–45 years
• Broadest available protection against HPV-related cancers and genital warts
Gardasil 4 (Quadrivalent)
• Strains covered: HPV 6, 11, 16, 18
• Age range: 9–26 years
• Also prevents genital warts
Cervarix (Bivalent)
• Strains covered: HPV 16, 18
• Age range: 9–25 years
• Targets the two main cancer-causing HPV strains
CERVAVAC (Made in India – Bivalent)
• Strains covered: HPV 16, 18
• Age range: 9–26 years
• Developed by the Serum Institute of India, the most affordable option available
• Launched in 2023 as India’s first indigenously developed HPV vaccine
HPV Vaccine Dosing Schedule: 2-Dose vs 3-Dose
The number of doses you need depends on your age when you receive your first shot. The younger you are when you are vaccinated, the stronger your immune response and the fewer doses you will need.
2-Dose Schedule (Ages 9–14)
- Dose 1: Day 0 (start date)
- Dose 2: 6–12 months after Dose 1
Children in this age group require only two doses because their immune response is stronger.
3-Dose Schedule (Ages 15 and Older)
- Dose 1: Day 0 (start date)
- Dose 2: 1–2 months after Dose 1
- Dose 3: 6 months after Dose 1
The CDC recommends routine vaccination at ages 11 or 12 (beginning as early as age 9), well before potential exposure to HPV. Immunocompromised individuals aged 9–26 require three doses regardless of their age at first vaccination.
Note on single-dose schedules: As of early 2026, 89 countries, including the United States, have adopted a single-dose schedule for national immunisation programmes, particularly for Gavi-eligible low-income countries. Multi-dose schedules remain standard in India’s private market.
Why Is the HPV Vaccine Not Recommended After Age 26?
This is one of the most common questions about the HPV vaccine. The answer lies in biology and health economics.
The CDC’s Advisory Committee on Immunisation Practices (ACIP) does not recommend routine HPV vaccination for adults over 26 for the following reasons:
1. Prior Exposure Reduces Benefit
Most sexually active adults have already been exposed to one or more HPV strains by their mid-20s. Since the vaccine prevents infection but cannot treat existing HPV, its protective benefit is significantly lower in this age group.
2. Limited Cost-Effectiveness at the Population Level
A landmark study by Harvard T.H. Chan School of Public Health, published in PLOS Medicine, found that vaccinating adults beyond age 26 provides limited health benefit at the population level at a substantial cost. The study modelled HPV-associated cancer and genital wart outcomes across multiple age-group scenarios.
3. FDA Approval Up to Age 45 – With Nuance
The FDA has approved Gardasil 9 for use up to age 45. Adults aged 27–45 are encouraged to make an individual decision with their doctor. As the ACIP guidelines note, individuals in this age group at risk for new HPV infection can still benefit through shared clinical decision-making.
Bottom line: the vaccine is not banned after 26, it simply has the highest impact when given early. If you are over 26 and unvaccinated, speak to your doctor about whether it makes sense for your personal situation.
HPV Vaccine Side Effects: What to Expect
Extensive post-market safety surveillance confirms that HPV vaccines are safe and well-tolerated. TheCDC’s monitoring programme, which has tracked over 15,000 participants in pre-licensure trials for Gardasil 9, found no serious adverse events linked to HPV vaccination.
Common side effects (mild and temporary):
• Pain, redness, or swelling at the injection site (most common, reported by 20–90% of recipients)
• Mild fever (10–13% of recipients)
• Headache, fatigue, or mild nausea
• Dizziness or brief fainting
Sit for 15 minutes post-vaccination as a precaution. These side effects are a sign your immune system is responding normally. Serious allergic reactions are extremely rare. The vaccine is not recommended during pregnancy, but there is no evidence linking it to adverse outcomes if given inadvertently.
Over 15 years of post-market safety data from tens of millions of doses worldwide have confirmed that HPV vaccines are among the safest vaccines ever deployed at scale.
Symptoms of Cervical Cancer: Warning Signs to Know
Early-stage cervical cancer typically has no symptoms — which is why regular screening is so critical. Symptoms usually appear only when cancer has progressed. Common warning signs include:
• Abnormal vaginal bleeding (between periods, after sex, or after menopause)
• Unusual vaginal discharge (watery, bloody, or with a strong odour)
• Pelvic pain or pain during sexual intercourse
• Lower back or leg pain (more common in advanced stages)
• Unexplained weight loss or fatigue in later stages
• Difficulty urinating or blood in urine (advanced stage)
If you experience any of these symptoms, consult a gynaecologist immediately. Symptoms alone are not diagnostic, but early medical evaluation is essential.
How to Prevent Cervical Cancer: Preventive Measures
- Get the HPV Vaccine – As Early as Possible: The single most effective step. Vaccinate girls and boys aged 9–14 for maximum protection (2 doses). If you missed the window, vaccination up to age 45 may still be beneficial; ask your doctor.
- Get Regular Cervical Cancer Screening: Begin screening at age 21. A Pap smear every 3 years (or HPV DNA test every 5 years) detects precancerous cells early, when treatment is most effective. Vaccination does not replace screening.
- Practice Safe Sex: Using barrier contraception consistently reduces HPV transmission risk. Fewer lifetime sexual partners lowers cumulative HPV exposure.
- Quit Smoking: Smoking weakens the immune system’s ability to clear HPV infections and is an independent risk factor. Women who smoke are about twice as likely to develop cervical cancer.
- Seek Regular Gynaecological Care: Annual check-ups and open communication with your gynaecologist allow early detection of any abnormalities. Women with HIV or other immunocompromising conditions need more frequent screening.
HPV Vaccine in India: Availability and Cost in Hyderabad
India introduced CERVAVAC, the country’s first home-grown HPV vaccine, by the Serum Institute of India in 2023. As of 2025, India’s national immunisation programme is planned to include HPV vaccination for adolescent girls aged 9–14.
HPV vaccine costs in Hyderabad vary by brand and facility type:
• CERVAVAC (Made in India): ₹1,400 – ₹2,500 per dose in private clinics; free or ₹0–300 at government centres
• Cervarix: ₹3,000 – ₹3,500 per dose
• Gardasil 4: approximately ₹3,927 per dose
• Gardasil 9: approximately ₹10,850 per dose
Most individuals aged 9–14 require 2 doses (total: ₹2,800–₹8,000 depending on brand). Those aged 15 and above require 3 doses. Government hospitals in Hyderabad and Telangana may offer CERVAVAC free or at minimal cost for eligible adolescent girls under pilot programmes.
HPV Vaccination Does Not Replace Screening
The HPV vaccine and cervical cancer screening work best together, not as alternatives. The WHO’s global 90–70–90 strategy for eliminating cervical cancer by 2030 requires: 90% of girls vaccinated by age 15, 70% of women screened by age 35 and 45, and 90% of women with cervical disease receiving treatment.
Current vaccines do not cover all high-risk HPV strains; Gardasil 9 covers 9 types, but over a dozen high-risk strains exist. Regular Pap smears or HPV DNA tests remain the safety net for detecting precancerous changes caused by strains not covered by the vaccine.
Recommended screening schedule: Begin at age 21. Pap smear every 3 years, or HPV DNA test every 5 years if results are normal. Women with HIV or other immune conditions should be screened more frequently.
FAQs
Can the HPV vaccine prevent cervical cancer?
Yes. Girls vaccinated before age 17 have up to 90% lower risk of cervical cancer. Scotland’s 2024 registry data found zero cervical cancer cases in women vaccinated at ages 12–13. In India, if 90% of eligible girls are vaccinated, HPV 16 and 18 infections could fall by 97% over 50 years.
What is the HPV vaccine 3-dose schedule?
For those aged 15 and above: Dose 1 at Day 0, Dose 2 at 1–2 months, Dose 3 at 6 months. Children aged 9–14 need only 2 doses spaced 6–12 months apart; their immune response is stronger at a younger age.
Why is the HPV vaccine not recommended after 26?
Because most sexually active adults have already been exposed to HPV, the vaccine’s benefit is reduced. It prevents infection; it cannot treat one already present. Adults aged 27–45 can still be vaccinated with Gardasil 9 after consulting their doctor, especially those with limited prior exposure.
What HPV vaccine types are available in India?
Four vaccines are approved in India: Gardasil 9 (9 strains, ages 9–45), Gardasil 4 (4 strains, ages 9–26), Cervarix (2 strains, ages 9–25), and CERVAVAC (2 strains, ages 9–26). CERVAVAC is India’s own vaccine by the Serum Institute, used in the national free vaccination programme.
What is the HPV vaccine cost in Hyderabad?
CERVAVAC costs ₹1,400–₹2,500 per dose privately, and is free at government centres for eligible girls. Cervarix: ₹3,000–₹3,500. Gardasil 4: ~₹3,927. Gardasil 9: ~₹10,850. Total cost for a full series ranges from ₹2,800 (2 doses of CERVAVAC) to over ₹30,000 (3 doses of Gardasil 9). Confirm current prices with your healthcare provider.
What are the side effects of the HPV vaccine?
Mild and temporary: soreness at the injection site, mild fever, headache, or fatigue. Brief dizziness is possible; sit for 15 minutes after the shot. Serious adverse effects are extremely rare. Over 15 years of global safety data confirm no link to serious health conditions.
What are the symptoms of cervical cancer?
Early-stage cervical cancer often has no symptoms. Warning signs include abnormal vaginal bleeding, unusual discharge, pelvic pain, or pain during sex. These typically appear in later stages, which is why regular screening starting at age 21 is essential, even if you feel fine.
Is the HPV vaccine free in India?
Yes, as of 2025. India’s national programme offers free HPV vaccination to approximately 11.5 million girls aged 14 at government facilities. CERVAVAC, India’s own vaccine, is used in this programme. Private clinics charge ₹1,400–₹10,850 per dose depending on the brand.
What is the shot or injection to prevent cervical cancer?
The HPV vaccine is available in India as CERVAVAC, Gardasil, and Cervarix. It is an intramuscular injection given in the upper arm in 2 or 3 doses, depending on age. It is the only vaccine in the world that directly prevents cancer.