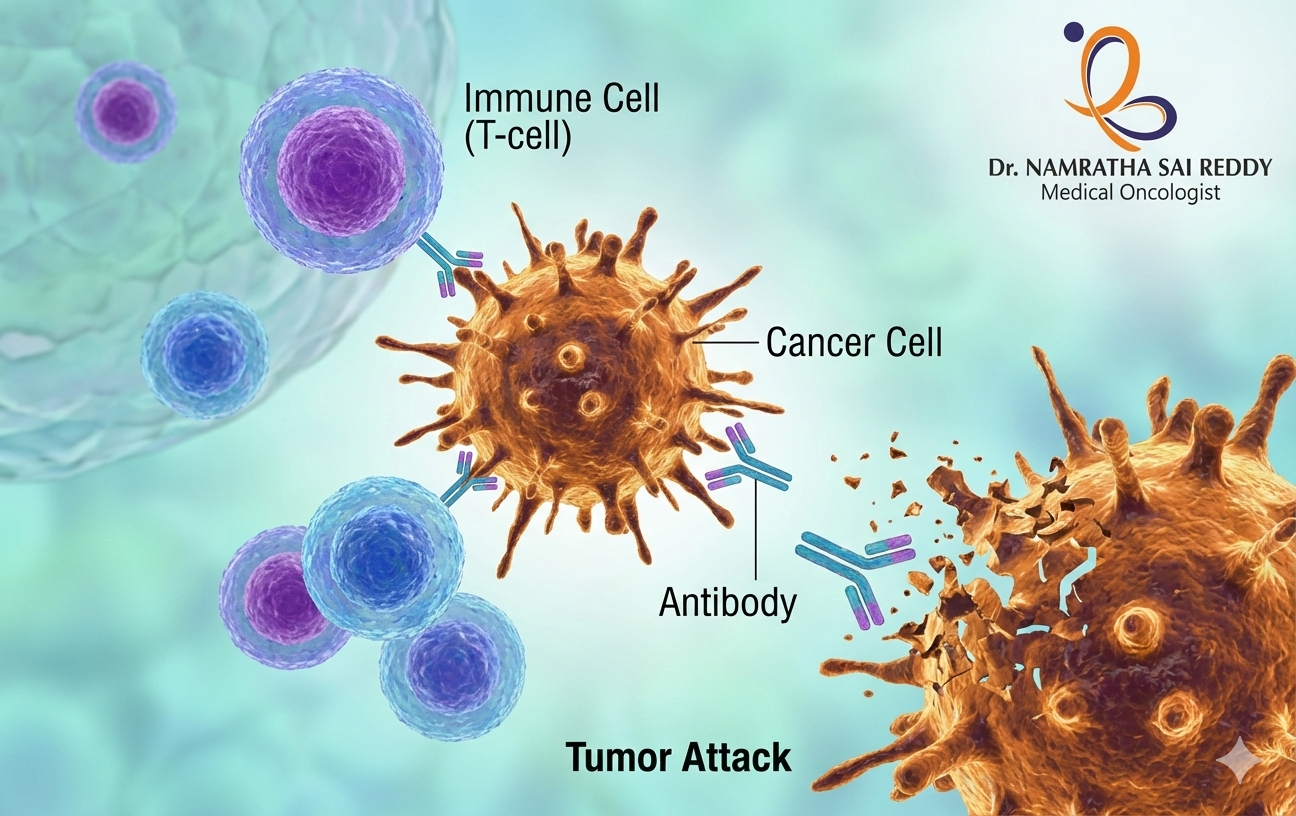
Cancer care has undergone a profound transformation in the last decade, and immunotherapy is at the centre of this change. Unlike traditional treatments that directly target tumors, immunotherapy works by strengthening the body’s own immune defenses against cancer. This shift has opened new possibilities for patients with advanced, recurrent, or treatment-resistant cancers.
As research progresses, doctors are learning how to use immunotherapy drugs more precisely and safely. In this blog, we explore the immunotherapy meaning, how treatment is given, its effectiveness, costs in India, and what patients should realistically expect from this rapidly evolving approach to cancer care.
What Is Immunotherapy?
The immunotherapy meaning refers to treatments that help your immune system recognise and fight cancer. Your immune system is designed to detect abnormal cells, including cancer cells, and destroy them before they cause harm.
Cancer becomes dangerous when it learns to hide from immune detection. Through complex signalling pathways, tumours can suppress immune responses and continue growing unchecked. Immunotherapy of cancer is treated with medicines that reverse this immune suppression.
Instead of attacking cancer cells directly, immunotherapy treatment empowers immune cells to do their job more effectively. This approach often leads to more targeted cancer control with less damage to healthy tissue compared to traditional therapies.
How Does Immunotherapy Work?
Understanding how immunotherapy works helps explain why outcomes can vary between patients. Immunotherapy targets the interaction between cancer cells and immune cells rather than the tumour itself.
Cancer cells often produce signals that tell immune cells to stop attacking. Immunotherapy cancer drugs interrupt these signals, allowing immune cells to stay active and focused on destroying cancer.
Key mechanisms include:
- Enhancing immune cell activation
- Removing immune system “brakes”
- Helping immune cells recognise cancer markers
- Supporting immune memory for long-term control
Because this process depends on your immune system, response rates differ. This variability explains why is immunotherapy effective for some patients and less effective for others.
Types of Immunotherapy Used in Cancer Treatment
There are several types of immunotherapy currently approved for cancer care. Each type works differently and is chosen based on cancer type, stage, and immune markers.
Types of immunotherapy include:
- Checkpoint inhibitors
- Adoptive cell therapy (T-cell transfer therapy)
- Monoclonal antibody therapy
- Cancer vaccines
- Immune system modulators
These immunotherapy drugs may be used alone or combined with other treatments such as chemotherapy or targeted therapy. Selection is always personalised to maximise benefit and reduce risk.
Checkpoint Inhibitors
Checkpoint inhibitors are among the most widely used immunotherapy cancer drugs today. They help immune cells called T cells remain active against cancer.
Normally, checkpoint proteins prevent T cells from attacking healthy tissue. Cancer exploits these checkpoints to shut down immune responses. Immunotherapy drugs known as checkpoint inhibitors block this shutdown.
By keeping T cells active, these drugs allow sustained immune attacks on tumours. Checkpoint inhibitors have shown success in cancers such as lung cancer, melanoma, kidney cancer, and some gastrointestinal cancers.
Adoptive Cell Therapy (T-Cell Transfer Therapy)
Adoptive cell therapy involves modifying a patient’s immune cells in a laboratory. These enhanced cells are then returned to the body to fight cancer more effectively.
Main types include:
- CAR T-cell therapy, where T cells are engineered to recognise cancer
- Tumour-infiltrating lymphocytes (TILs) selected from tumour tissue
- This highly specialised immunotherapy procedure is mainly used for blood cancers and select solid tumours. While powerful, it requires advanced infrastructure and close monitoring.
Monoclonal Antibody Therapy
Monoclonal antibodies are lab-engineered proteins designed to attach to specific cancer markers. Once attached, they help the immune system destroy cancer cells.
Some monoclonal antibodies:
- Block cancer growth signals
- Flag cancer cells for immune attack
- Deliver toxic or radioactive substances directly into cancer cells
These treatments are often categorised as immunotherapy drugs and targeted therapies. They play a major role in breast cancer, colorectal cancer, and lymphoma.
Cancer Vaccines
Cancer vaccines are different from vaccines that prevent infections. Instead, they train the immune system to recognise cancer cells already present in the body.
These vaccines expose immune cells to cancer-specific markers. Once trained, immune cells can seek out and destroy cancer cells more efficiently.
Cancer vaccines are still evolving, but they represent a promising area of immunotherapy treatment, especially when combined with other immune-based approaches.
Immune System Modulators (Immunomodulators)
Immune system modulators broadly enhance immune responses. Because they act in different ways, they are sometimes called nonspecific immune agents.
Examples include:
- Cytokines that coordinate immune attacks
- Drugs that increase immune cell production
- Agents that block the tumour blood supply
Some treatments, such as BCG for bladder cancer, are given as a localised cancer injection. These therapies have been used successfully for decades in specific cancers.
How Is Immunotherapy Done?
Patients often ask, how immunotherapy is done in practice. The answer depends on the specific drug and cancer type.
Before starting treatment, doctors perform tests to evaluate immune markers and overall health. This ensures the chosen immunotherapy procedure is appropriate and safe.
Immunotherapy may be given as:
- Intravenous infusions
- Oral medications
- Topical applications
- Targeted cancer injection
- Bladder instillation therapy
Immunotherapy Procedure: Step-by-Step Overview
The immunotherapy procedure typically follows a structured plan designed to balance effectiveness and safety.
| Step | What Happens |
| Evaluation | Cancer testing and immune profiling |
| Planning | Selection of suitable immunotherapy drugs |
| Treatment | Infusion, pill, or injection |
| Monitoring | Blood tests and imaging |
| Cycles | Treatment with scheduled breaks |
Treatment may be continuous or cyclical. Rest periods allow the body to recover while maintaining immune activity.
Is Immunotherapy Effective?
A common question looms about the effectiveness of immunotherapy. The answer is no, but its impact can be significant for the right patients.
Effectiveness depends on:
- Cancer type and stage
- Tumor genetics
- Immune system strength
- Previous treatments
Some patients experience dramatic and long-lasting responses. Others may see modest benefit or none at all.
Immunotherapy Success Rate for Cancer
There is no single immunotherapy success rate for cancer. Success varies widely across cancer types and patient populations.
For certain cancers, immunotherapy has doubled or tripled survival rates compared to older treatments. In others, it works best as part of a combination therapy.
Ongoing research continues to refine patient selection to improve outcomes.
Can Immunotherapy Cure Stage 4 Cancer?
Many patients ask this question. In most cases, immunotherapy does not provide a complete cure.
However, it can:
- Shrink tumours significantly
- Slow disease progression
- Improve survival
- Enhance quality of life
In some patients, advanced cancer becomes a manageable chronic condition. This represents a major shift in cancer care.
Immunotherapy Cost in India
Cost is a major concern for patients. Immunotherapy cost in India varies based on several factors.
| Factor | Impact on Cost |
| Drug type | Imported drugs cost more |
| Duration | Longer treatment increases cost |
| Cancer type | Combination therapy raises cost |
| Hospital | Public vs private setting |
Doctors help patients balance potential benefit, affordability, and safety when planning treatment.
Recovery and Outlook
Recovery during immunotherapy differs from traditional treatments. Many patients maintain better daily functioning compared to chemotherapy.
Side effects are usually immune-related and may include fatigue, skin changes, or inflammation. Early reporting allows timely management.
Long-term outlook continues to improve as newer immunotherapy drugs are developed.
When Should You Call Your Healthcare Provider?
Patients should contact their oncologist if symptoms worsen or new side effects appear. Prompt evaluation helps prevent complications.
Questions to discuss include:
- How long will treatment continue?
- How will the response be monitored?
- Are newer options available?
- What lifestyle changes are recommended?
Where Immunotherapy Is Headed Next
Immunotherapy is no longer an emerging concept; it is an evolving pillar of modern cancer care. Ongoing advancements are improving how immunotherapy drugs are designed, combined, and personalised for individual patients. Researchers are refining types of immunotherapy to increase response rates, reduce side effects, and extend the durability of results.
New biomarkers, smarter drug combinations, and better delivery methods are steadily improving the immunotherapy success rate for cancer. As these innovations move from clinical trials into routine care, immunotherapy will continue to redefine how cancer is treated, shifting the focus toward longer survival, improved quality of life, and more precise, immune-driven cancer control.
FAQs
What is immunotherapy?
It is a treatment that uses the immune system to fight cancer.
Is immunotherapy safer than chemotherapy?
It usually causes fewer side effects but can still have risks.
How long does immunotherapy treatment last?
Treatment duration varies from months to years.
Does everyone respond to immunotherapy?
No, response depends on cancer biology.
Can immunotherapy be combined with chemotherapy?
Yes, combination therapy is common.
Is immunotherapy painful?
Most patients tolerate it well.